NIH researchers achieved tumor shrinkage in three of seven
patients with colorectal cancers
BETHESDA, Md., July 11,
2024 /PRNewswire/ --Early findings from a small
clinical trial provide evidence that a new cellular immunotherapy
approach may be effective in treating metastatic solid tumors. In
the trial, researchers from the National Institutes of Health (NIH)
genetically engineered normal white blood cells, known as
lymphocytes, from each patient to produce receptors that recognize
and attack their specific cancer cells. These initial findings are
from people with metastatic colorectal cancer who had already
undergone multiple earlier treatments. The personalized
immunotherapy shrank tumors in some patients and was able to keep
the tumors from regrowing for up to seven months. The findings were
published July 11, 2024, in Nature
Medicine.
One form of cellular immunotherapy, chimeric antigen
receptor (CAR) T-cell therapy, has already been shown to be
effective against some blood cancers, and another, called
tumor-infiltrating lymphocyte (TIL) therapy, has proven to be
effective against metastatic melanoma. However, to date, a cellular
therapy that's effective against any other solid cancers has been
elusive, according to Steven A.
Rosenberg, M.D., Ph.D., of NCI's Center for Cancer Research
(CCR), who co-led the study with Maria
Parkhurst, Ph.D., of CCR's Surgery Branch.
"The fact that we can take a growing metastatic solid cancer and
get it to regress shows that the new cellular immunotherapy
approach has promise," Dr. Rosenberg said. "However, it's important
to understand that these findings are preliminary and that the
approach needs to be further refined and tested in more types of
solid cancers."
The new approach overcomes two challenges in
cellular immunotherapy: how to produce large numbers of T
cells that can recognize cancer cells specifically, and how to
boost the ability of modified T cells to multiply once they've been
returned to the patient.
For each patient in the study, Dr. Rosenberg and his
colleagues collected lymphocytes present in the patient's tumors.
They then used sophisticated molecular characterization techniques
to identify and isolate receptors on those lymphocytes, called
T-cell receptors, that recognized specific changes in each
patient's tumor. After genetically sequencing those receptors, they
then used a retrovirus to insert the genes for the receptor into
normal lymphocytes collected from each patient's circulating
blood.
The genetically modified lymphocytes were then multiplied into
the hundreds of millions in the laboratory and infused back into
the patients, where they expressed the tumor-specific T-cell
receptors and continued to multiply.
"By taking the natural T-cell receptors that are present in
a very small number of cells and putting them into normal
lymphocytes for which we have enormous numbers—a million in every
thimbleful of blood—we can generate as many cancer-fighting cells
as we want," Dr. Rosenberg explained.
As part of a larger phase 2 trial, seven patients with
metastatic colon cancer were treated with the experimental
personalized cellular immunotherapy. All seven received
several doses of the immunotherapy drug pembrolizumab before the
cell therapy and another immunotherapy drug called IL-2 afterward.
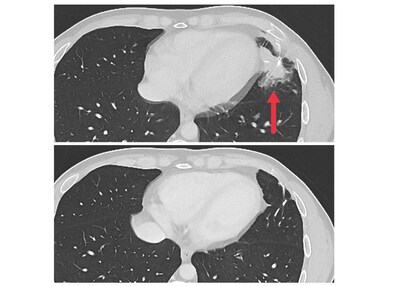
Three patients had substantial shrinkage of metastatic tumors in
the liver, lung, and lymph nodes that lasted for four to seven
months. The median time to disease progression was 4.6 months.
Dr. Rosenberg noted that, of the three patients who
responded to the treatment, two had received T-cell receptors
derived from cytotoxic T cells, which are primarily responsible for
killing diseased cells. Dr. Rosenberg said his research team is
exploring how to put the T cell receptors into subtypes of normal
lymphocytes to improve their reactivity.
Colon cancer is just one of many solid tumors the researchers
are studying. The trial is still ongoing and includes patients with
different types of solid cancers.
"It's just the very beginning of converting normal lymphocytes
into cells capable of treating the common solid cancers,"
Dr. Rosenberg said. "What this study shows is that it's
possible. Once you know it's possible, you work to improve it."
About the National Cancer Institute (NCI): NCI leads the
National Cancer Program and NIH's efforts to dramatically reduce
the prevalence of cancer and improve the lives of people with
cancer. NCI supports a wide range of cancer research and training
extramurally through grants and contracts. NCI's intramural
research program conducts innovative, transdisciplinary basic,
translational, clinical, and epidemiological research on the causes
of cancer, avenues for prevention, risk prediction, early
detection, and treatment, including research at the NIH Clinical
Center—the world's largest research hospital. Learn more about
NCI's intramural research from the Center for Cancer Research and
the Division of Cancer Epidemiology and Genetics. For more
information about cancer, please visit the NCI website at
cancer.gov or call NCI's contact center at 1-800-4-CANCER
(1-800-422-6237).
About the National Institutes of Health (NIH): NIH, the
nation's medical research agency, includes 27 Institutes and
Centers and is a component of the U.S. Department of Health and
Human Services. NIH is the primary federal agency conducting and
supporting basic, clinical, and translational medical research, and
is investigating the causes, treatments, and cures for both common
and rare diseases. For more information about NIH and its programs,
visit nih.gov.
 View original content to download
multimedia:https://www.prnewswire.com/news-releases/immunotherapy-approach-shows-potential-in-some-people-with-metastatic-solid-tumors-302195265.html
View original content to download
multimedia:https://www.prnewswire.com/news-releases/immunotherapy-approach-shows-potential-in-some-people-with-metastatic-solid-tumors-302195265.html
SOURCE NATIONAL CANCER INSTITUTE